- Adrenal gland
- Minimally Invasive Adrenal Surgery
-
JungHak Kwak, Kyu Eun Lee
-
Endocrinol Metab. 2020;35(4):774-783. Published online December 23, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.404
-
-
5,111
View
-
155
Download
-
8
Web of Science
-
8
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
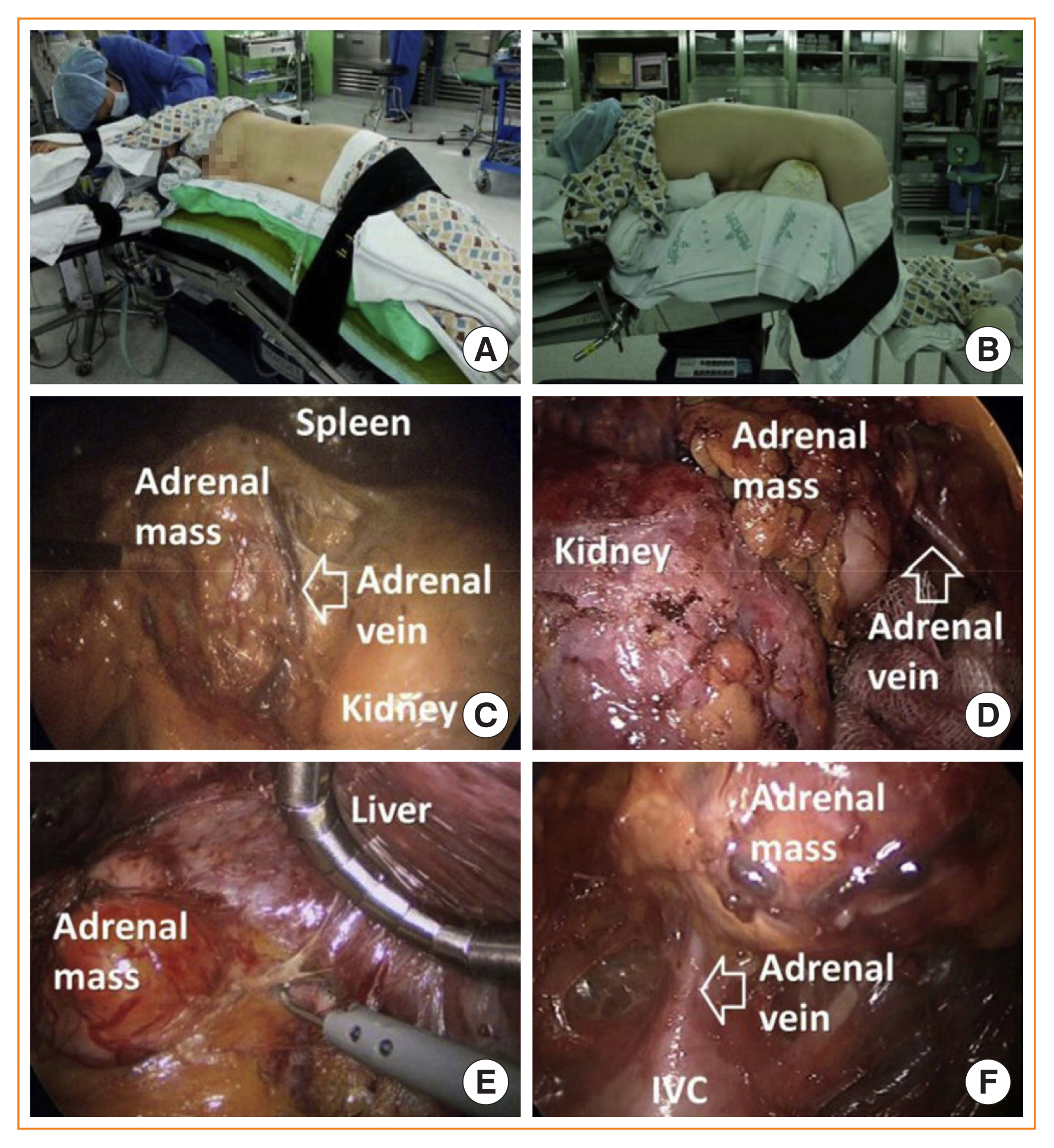
- Since the introduction of minimally invasive surgery, laparoscopic adrenalectomy has become the main treatment option for adrenal masses. Various studies have reported that laparoscopic adrenalectomy showed fewer postoperative complications and faster recovery than conventional open adrenalectomy. Laparoscopic adrenalectomy can be performed through either the transperitoneal approach or the retroperitoneoscopic approach, which are widely used in most adrenal surgical procedures. Furthermore, with the development of minimally invasive surgery, organ-sparing adrenalectomy has recently emerged as a way to conserve functional adrenal gland tissue. According to recent data, organ-sparing adrenalectomy shows promising surgical, functional, and oncological outcomes including less intraoperative blood loss, maintenance of adrenal function, and low recurrence. Partial adrenalectomy was initially proposed for bilateral adrenal tumors in patients with hereditary disease to avoid chronic adrenal insufficiency. However, it has also gained popularity for the treatment of unilateral adrenal disease involving a small adrenal tumor because even patients with a unilateral adrenal gland may develop adrenal insufficiency in stressful situations. Therefore, partial adrenalectomy has become increasingly common to avoid lifelong steroid replacement and recurrence in most cases, especially in bilateral adrenal disease. This review article evaluates the current evidence on minimally invasive adrenalectomy and organ-preserving partial adrenalectomy.
-
Citations
Citations to this article as recorded by  - Treating Primary Aldosteronism-Induced Hypertension: Novel Approaches and Future Outlooks
Nathan Mullen, James Curneen, Padraig T Donlon, Punit Prakash, Irina Bancos, Mark Gurnell, Michael C Dennedy
Endocrine Reviews.2024; 45(1): 125. CrossRef - Modified versus three-level technique of retroperitoneal laparoscopic adrenalectomy for all patients with adrenal lesions ≤ 6cm: a retrospective, case-controlled study
Minxiong Hu, Yangbiao Wu, Xiao Xu, Wenchao Cai, Jiangui Lin, Wanghai Cai, Honghong Pan, Zesong Yang, Liefu Ye, Jinfeng Wu
Frontiers in Endocrinology.2024;[Epub] CrossRef - Ultrasound-guided Transversus Abdominis Plane Block is Effective as Laparoscopic Trocar site infiltration in Postoperative Pain Management in Patients Undergoing Adrenal Surgery
Giuseppe Cavallaro, Sergio Gazzanelli, Angelo Iossa, Francesco De Angelis, Alessia Fassari, Alessandra Micalizzi, Luigi Petramala, Daniele Crocetti, Francesco Circosta, Antonio Concistrè, Claudio Letizia, Giorgio De Toma, Andrea Polistena
The American Surgeon™.2023; 89(11): 4401. CrossRef - Outcome of Partial Adrenalectomy in MEN2 Syndrome: Personal Experience and Systematic Review of Literature
Priscilla Francesca Procopio, Francesco Pennestrì, Carmela De Crea, Nikolaos Voloudakis, Rocco Bellantone, Marco Raffaelli
Life.2023; 13(2): 425. CrossRef - Impact of Current Technology in Laparoscopic Adrenalectomy: 20 Years of Experience in the Treatment of 254 Consecutive Clinical Cases
Giovanni Conzo, Renato Patrone, Luigi Flagiello, Antonio Catauro, Alessandra Conzo, Chiara Cacciatore, Federico Maria Mongardini, Giovanni Cozzolino, Rosetta Esposito, Daniela Pasquali, Giuseppe Bellastella, Katherine Esposito, Ludovico Docimo
Journal of Clinical Medicine.2023; 12(13): 4384. CrossRef - Safety and effectiveness of minimally invasive adrenalectomy versus open adrenalectomy in patients with large adrenal tumors (≥5 cm): A meta-analysis and systematic review
Lijian Gan, Chunyang Meng, Kangsen Li, Lei peng, Jinze Li, Ji Wu, Yunxiang Li
International Journal of Surgery.2022; 104: 106779. CrossRef - Retroperitoneal laparoscopic partial adrenalectomy (RLPA) for 20-40 mm nonfunctional adrenal tumors in the day surgery mode
Xuwen Li, Haibo Xi, Yue Yu, Wei Liu, Xiaoping Zhu, Zhixian Gong, Bin Fu, Gongxian Wang, Xiaochen Zhou
Frontiers in Endocrinology.2022;[Epub] CrossRef - Cirugía laparoscópica en incidentaloma suprarrenal para el cirujano general: serie de casos
Martín Adrián Bolívar-Rodríguez, Marcel Antonio Cázarez-Aguilar, Pedro Alejandro Magaña-Zavala, Francisco Magaña-Olivas, José Martín Niebla-Moreno
Revista Mexicana de Cirugía Endoscópica.2021; 22(1): 8. CrossRef
- Clinical Study
- Efficacy of Intraoperative Neuromonitoring in Reoperation for Recurrent Thyroid Cancer Patients
-
Jang-il Kim, Su-jin Kim, Zhen Xu, JungHak Kwak, Jong-hyuk Ahn, Hyeong Won Yu, Young Jun Chai, June Young Choi, Kyu Eun Lee
-
Endocrinol Metab. 2020;35(4):918-924. Published online December 23, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.778
-
-
3,904
View
-
102
Download
-
5
Web of Science
-
3
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The use of intraoperative neuromonitoring (IONM) in thyroid surgery to preserve recurrent laryngeal nerve (RLN) function has been widely accepted. We aimed to evaluate the usefulness of IONM in reoperation for recurrent thyroid cancer patients to help identify the RLN and prevent vocal cord palsy (VCP).
Methods
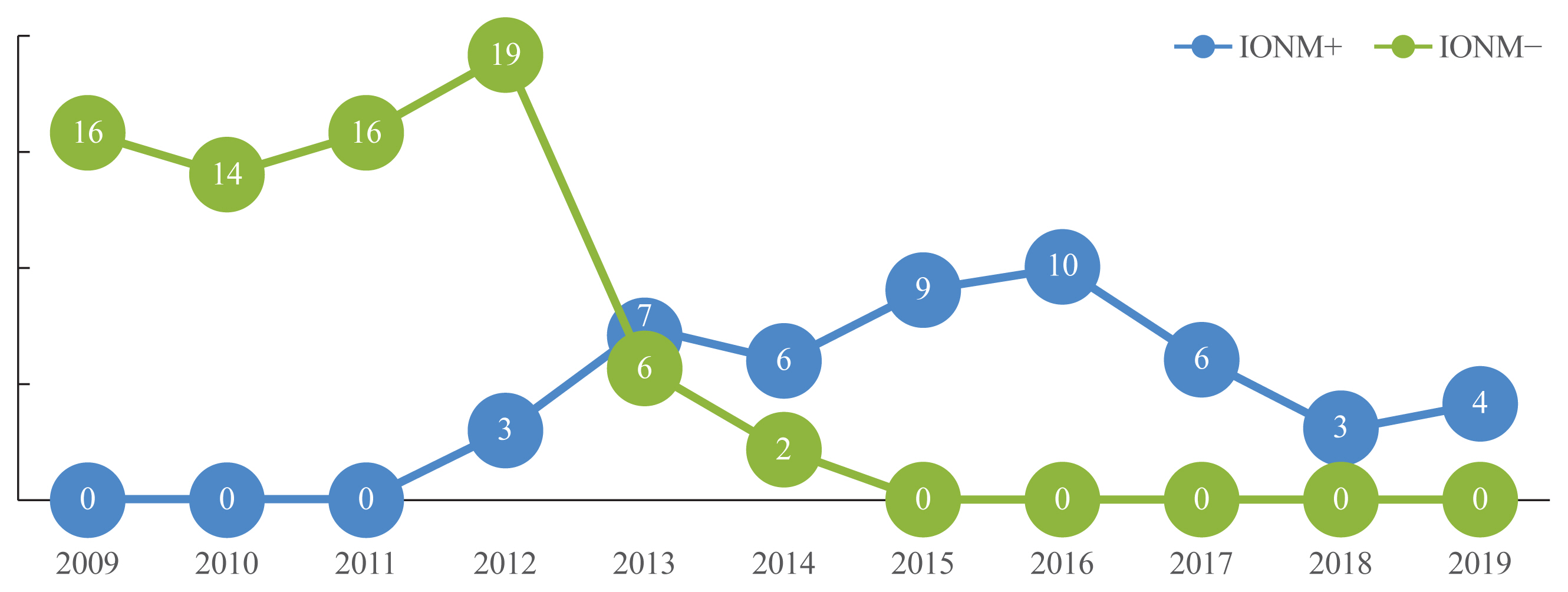
We analyzed 121 consecutive patients (with IONM group, 48 patients; without IONM group, 73 patients) who underwent reoperation for recurrent thyroid cancer after total thyroidectomy from January 2009 to March 2019 in our institution without VCP due to previous operations. Data including age, sex, number of previous operations, histologic subtype of the malignancy at the initial operation, operation time, RLNs at risk, difficulty of RLN identification, surgical procedure, VCP, and other postoperative complications were reviewed. Vocal cord movement evaluations were performed preoperatively and at 2 weeks postoperatively to evaluate RLN function. In patients with VCP, additional evaluations were performed. VCP exceeding 12 months after surgery was considered permanent VCP.
Results
VCP was observed in six (12.5%) and 16 (21.9%) patients with and without IONM (P=0.189). Transient and permanent VCP were found in three (6.3%) and three (6.3%) patients with IONM (P=0.098 and P=0.982, respectively) versus in 12 (16.4%) and four (5.5%) patients without IONM.
Conclusion
The incidence of transient VCP seems to be lower in reoperations with IONM; however, there was no statistical significances. Further study will be needed to ascertain the efficacy of IONM in reoperation for recurrent thyroid cancer patients.
-
Citations
Citations to this article as recorded by  - The learning curve for gasless transaxillary posterior endoscopic thyroidectomy for thyroid cancer: a cumulative sum analysis
Weisheng Chen, Shitong Yu, Baihui Sun, Cangui Wu, Tingting Li, Shumin Dong, Junna Ge, Shangtong Lei
Updates in Surgery.2023; 75(4): 987. CrossRef - Intraoperative neuromonitoring of the recurrent laryngeal nerve is indispensable during complete endoscopic radical resection of thyroid cancer: A retrospective study
Yang Fei, Yang Li, Feng Chen, Wen Tian
Laryngoscope Investigative Otolaryngology.2022; 7(4): 1217. CrossRef - The value of intraoperative nerve monitoring against recurrent laryngeal nerve injury in thyroid reoperations
Maowei Pei, Siqi Zhu, Chunjie Zhang, Guoliang Wang, Mingrong Hu
Medicine.2021; 100(51): e28233. CrossRef
|